CareTime has Revolutionized the way Home Care Agencies do EVV
Say Goodbye to Chasing after Claims and EVV Data!
- Ever wish you knew at which step your EVV and claims data was in the claims submission process?
- Do you prepare your claims, press a button, and spend time hunting it down to figure out why it wasn’t processed?
- Ultimately — do you submit your EVV claims and wonder where its gone?
No Need to Wonder Anymore.
|
EVV Feature |
CareTime |
Other EVV Software |
|---|---|---|
|
Comprehensive View of EVV |
|
|
|
Claims Data in a Single Dashboard |
|
|
|
Quick View Status of EVV Claims |
|
|
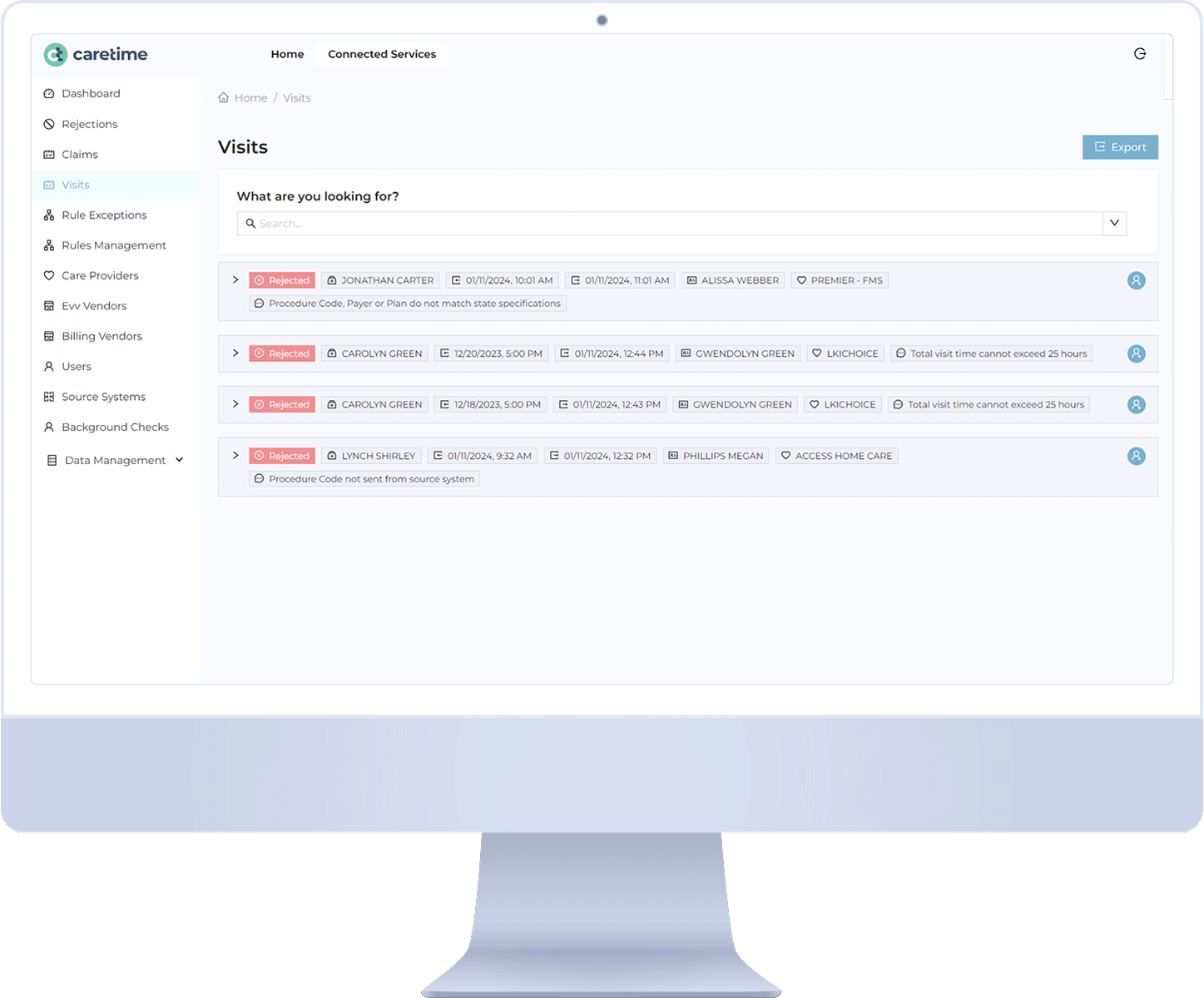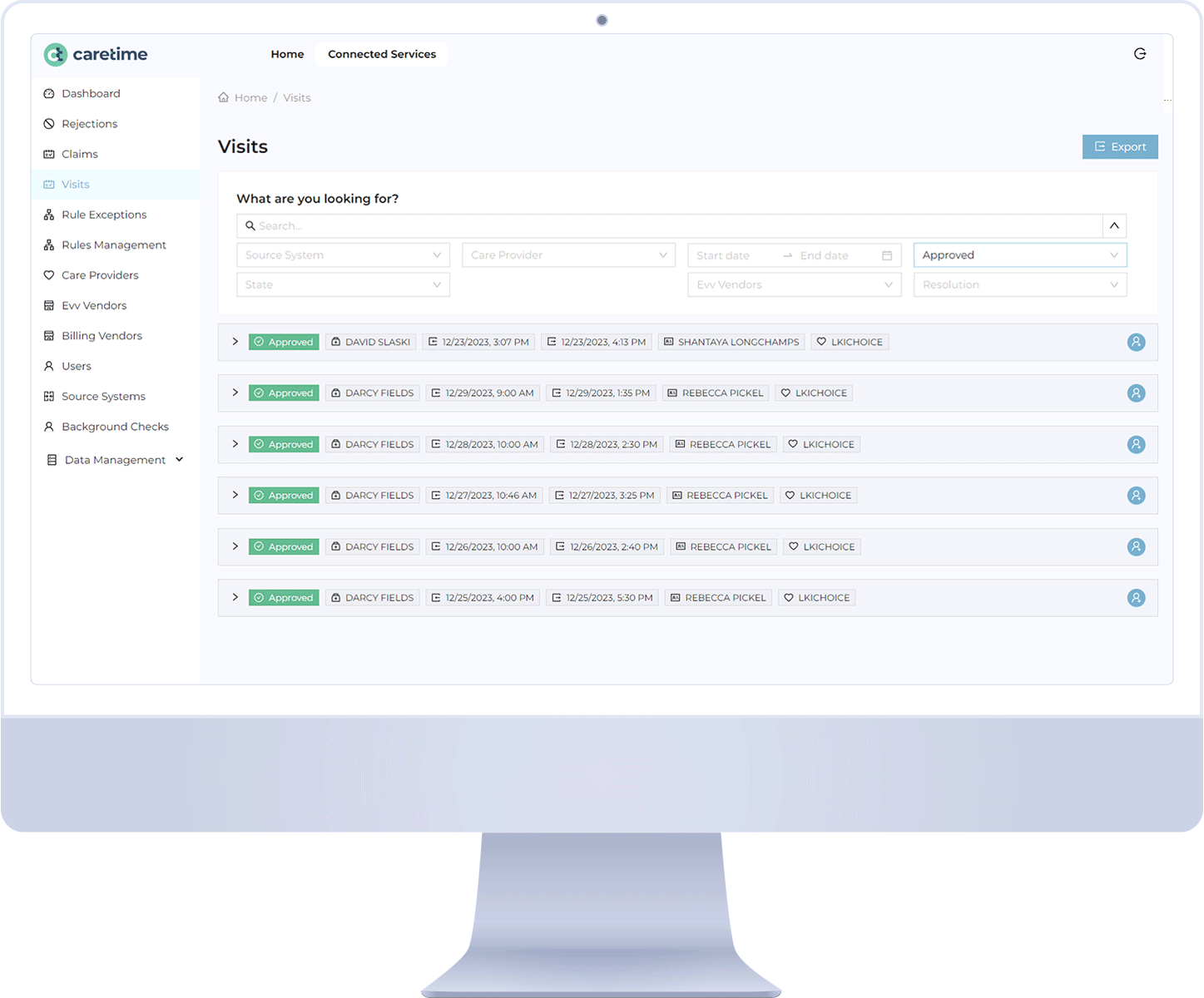
FEATURES FOR AGENCY OWNERS
CareTime’s Electronic Visit Verification (EVV)
and Telephony Software
CareTime’s multi-technology electronic visit verification solution is a compliant EVV system for providers. Our EVV uses GPS, cell phone, and telephony technologies. A few other features, like fixed-based and voice-bot, are available upon request.
- Multiple Technologies for EVV
- Visit Notes, Details, and Tasks
- Integrate with Other Software
- EVV: Track Visits and Duration Effortlessly
- Offline Visits: No Service Area Visits
- Multilingual: English and Spanish
- Voice Verification for Extra Security
- Creates Billing and Payroll Data Automatically
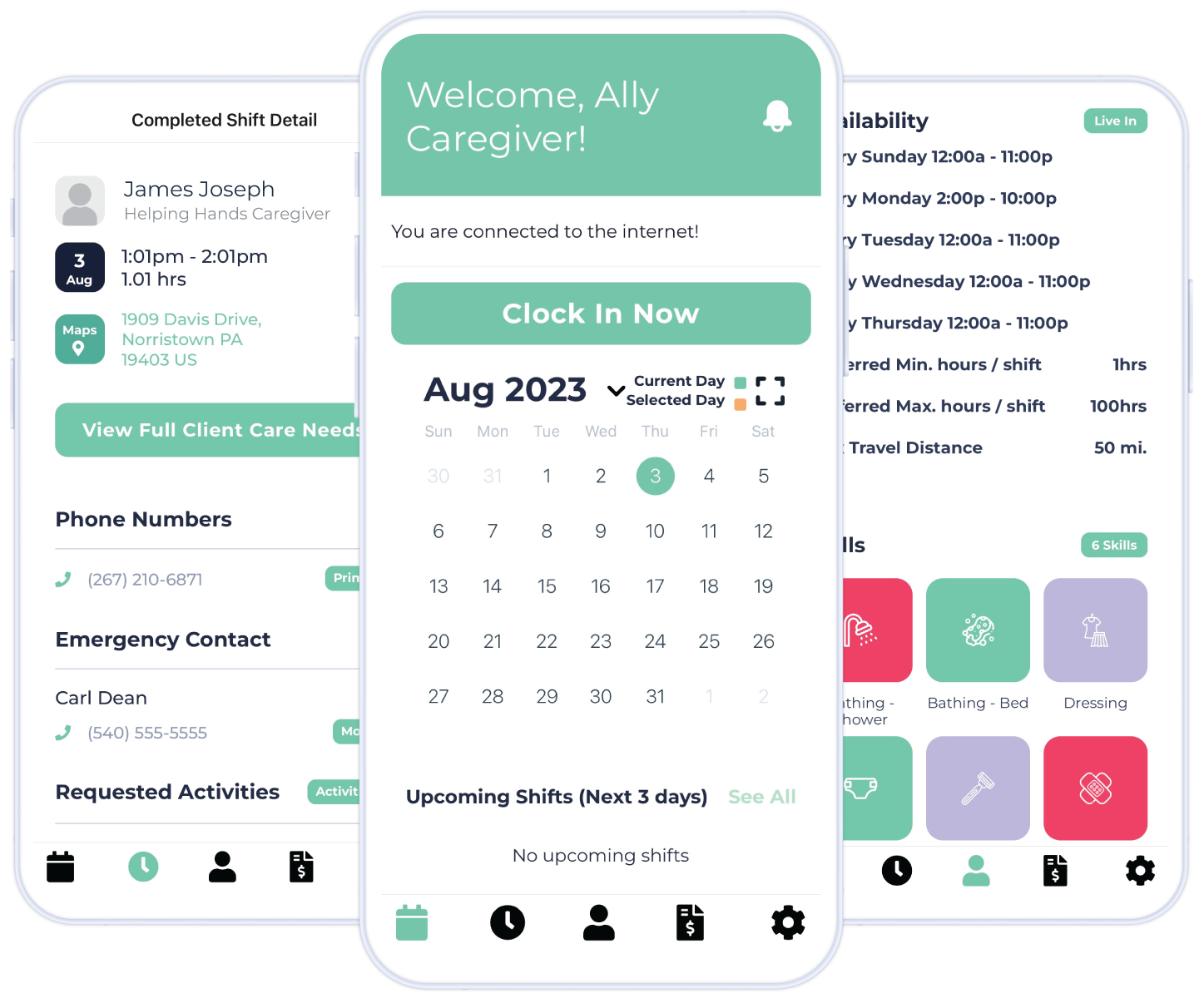
FEATURES FOR CAREGIVERS & FAMILIES
EVV Mobile App
- iOS and Android apps
- Easy clock in and clock out
- Create and review care notes
- Designate activity codes for specific services
- Receive notifications to the app
- Document care plan tasks
- Map driving directions to jobs
- Caregivers can review hours worked
- Offline visits using an in-home device and the app
WEBINAR RECORDING
Leveraging CareTime for Optimal EVV Visibility
Watch the On-Demand Webinar & Learn:
- The current state of EVV & claims data and the struggles agencies face
- Challenges connecting with aggregators
- Why an agency needs EVV visibility
- Insights from a customer who has been there - just like you
- How CareTime V3 transforms EVV visibility
- Glimpse at CareTime V3 portal
- Q&A

Who Benefits From Our EVV Software?

EVV for Providers & Consumer-Directed Care
Multi-technology, user-friendly electronic visit verification software created for providers and consumer directed care.

EVV for States
Our fully-capable and reliable system is built to be a state-compliant EVV. States can either use our system or request a customized EVV solution developed for their specific needs. CareTime has been approved and used in many states by thousands of users.

EVV for Payers & MCOs
Gain insights into the accuracy, expected reimbursements, and real-time visits with our EVV solution for payers.
Electronic Visit Verification, commonly referred to as EVV, is a technology-based system that verifies when and where home health care services are provided. This system is designed to ensure accuracy and reliability in the delivery of care services, particularly for those who are elderly, disabled, or require long-term care.
EVV systems work by using technology to record and verify key information about the services provided during a home health care visit. This can be done through various methods, including mobile applications, landline telephones, and fixed devices installed in the patient's home.
When a care provider arrives at a patient's home, they check-in using the EVV system, which records the time, date, and location of the visit. The same process is repeated when the visit ends. The system then transmits this information to a central database for verification and billing purposes.
EVV offers numerous benefits for both care providers and patients. For providers, it simplifies the process of documenting and verifying services, reducing the risk of errors and fraud. It also provides a reliable record of care, which can be used for quality assurance and compliance purposes.
For patients, EVV ensures that they receive the services they need, when they need them. It also provides a level of transparency and accountability, giving patients and their families peace of mind that their care is being properly managed.
The 21st Century Cures Act, enacted by the U.S. Congress in 2016, mandates the use of EVV for all Medicaid-funded personal care services and home health care services. However, the requirement of EVV for Medicare is not as straightforward.
As of now, the Centers for Medicare & Medicaid Services (CMS) does not require EVV for home health services under Medicare. However, this does not mean that EVV is irrelevant for Medicare beneficiaries. Many home health agencies that provide services to Medicare beneficiaries use EVV systems to ensure service delivery and streamline operations.
The Role of EVV in Medicare Advantage Plans
While EVV is not mandated for traditional Medicare, it plays a significant role in Medicare Advantage plans. Medicare Advantage plans are an alternative to traditional Medicare, offered by private companies approved by Medicare. These plans often include additional benefits, such as home health care services, that are not covered under traditional Medicare.
Many Medicare Advantage plans require the use of EVV for home health care services. This requirement ensures that beneficiaries receive the services they are entitled to and helps prevent fraudulent claims. Therefore, while EVV is not directly required by Medicare, it is a critical component of many Medicare Advantage plans.
Federal Regulations Surrounding EVV
The federal government has recognized the importance of EVV and has implemented regulations to ensure its widespread adoption. The 21st Century Cures Act, enacted in 2016, mandates EVV implementation for Medicaid-funded personal care services and home healthcare services. This legislation aims to curb fraud, promote accountability, and ultimately enhance the quality of care provided to Medicaid beneficiaries.
Under the 21st Century Cures Act, EVV systems must meet certain criteria to comply with federal regulations. These criteria include capturing the date, start time, end time, and location of the service, as well as the individual providing the service. By standardizing these data elements, the Act aims to create consistency and transparency in EVV implementation across different healthcare settings.
State-by-State EVV Requirements
While the federal government sets the groundwork for EVV, individual states have the autonomy to implement their own requirements. It's important for healthcare providers to familiarize themselves with the specific EVV requirements in the states they operate in. Each state may have slight variations in terms of implementation timelines, data elements to be collected, and penalties for non-compliance.
State-specific EVV requirements can pose challenges for multi-state healthcare providers, as they must ensure compliance with varying regulations. Some states may require additional data elements to be captured in the EVV system, such as caregiver qualifications or specific service tasks performed. Understanding these nuances is essential for healthcare organizations to tailor their EVV systems accordingly.
Read More About EVV

SOFTWARE FOR ALL HOME CARE MODELS
✓ Agency (W-2)
✓ Consumer-Directed Care
✓ Caregiver Registry (1099)
Power your home care agency with an all-in-one cloud-based desktop and mobile software solution that handles your business’s specific needs.
Get EVV Compliant in Minutes!
Curious, even just a bit? Schedule a meeting, it's worth a conversation.
Are you currently a CareTime user looking for support? Click here.






